3 Fascia Release Principles Every Practitioner Must Know
A practitioner-grade guide grounded in modern fascia science, neurophysiology, and hands-on clinical reality.
Why Fascia Release Matters for Pain, Performance, and Clinical Results
Practitioner Note: This article is part of our evidence-based fascia education series at the Fascia Training Institute. It is designed for chiropractors, physical therapists, manual therapists, and bodyworkers who want faster, longer-lasting results without using more force.
If pain does not resolve with muscle work, joint adjustments, or strengthening, it is rarely a technique failure.
It is most often a fascial system problem.
Over the last two decades, fascia research, including the work of Dr. Robert Schleip and colleagues, has fundamentally changed how we understand pain, movement restriction, and tissue adaptation. Fascia is no longer viewed as passive packing material. It is now recognized as a dynamic, responsive, neurologically active system.
Current research shows that fascia is:
- Contractile – it actively responds rather than passively stretches
- Highly innervated – functioning as a major sensory and interoceptive organ
- Hydration‑dependent -fluid dynamics determine tissue glide and adaptability
- Neurologically regulated -nervous system state directly influences tissue tone
When practitioners understand how fascia actually behaves, clinical outcomes become:
- faster
- easier to achieve
- longer‑lasting
This guide outlines the three non‑negotiable fascia release principles that must be present for meaningful change — regardless of modality, tool, or technique.
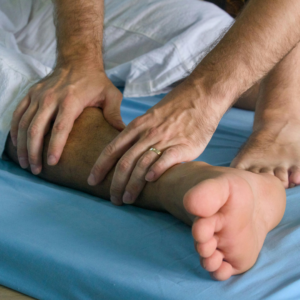
Principle #1: Fascia Releases Through Time and Safety – Not Force
Why the Traditional Model Fails
Many manual therapy approaches still rely on:
- more pressure
- faster strokes
- deeper digging
- pushing through resistance
While this may feel productive, it often triggers protective contraction rather than release.
The Fascia Science
Fascia contains smooth‑muscle‑like cells known as myofibroblasts. These cells respond to:
- sustained load
- slow deformation
- reduced threat signals
When pressure is applied too quickly or aggressively, the nervous system interprets threat. The result is increased tissue tone, guarding, and resistance.
What Works Instead
Effective fascia release relies on:
- slow, sustained contact (30–120 seconds) sink into the tissues
- gradual loading rather than sudden force
- practitioner stillness, regulation, and presence
Why this works: Slow pressure reduces sympathetic nervous system activation, allowing fascia to shift from protection into adaptability.
Practitioner Application
Before increasing pressure, ask:
Has the tissue accepted my contact?
If the client is holding their breath, bracing, or mentally withdrawing, the fascia will not release.

Principle #2: Hydration Changes Fascia Faster Than Stretching
Fascia Is a Fluid System
Fascia is a hydrated collagen matrix, not dry rope.
Healthy fascia:
- glides freely
- transmits force efficiently
- distributes load evenly
Dehydrated fascia:
- sticks and densifies
- restricts movement
- amplifies pain signals
- increases fatigue and compensation
The Key Insight
You are not stretching fascia.
You are changing fluid dynamics within the tissue.
How Fascial Hydration Happens Clinically
Hydration and glide improve through:
- slow shear forces
- compression and decompression cycles
- gentle oscillation
- sustained contact with micro‑movement
These principles align with modern fascia hydration research and nervous‑system‑based manual therapy approaches.
Less force + more time = more glide.
Practitioner Application
If tissue feels stuck or unresponsive:
- slow down
- reduce force
- wait for warmth, softening, or spreading sensation
These are objective hydration signs — not imagination.
Principle #3: Fascia Responds to Nervous System State First
The Missing Link in Most Manual Therapy
Fascia does not change in isolation.
It responds to the brain’s perception of safety.
Research highlights fascia as a primary sensory organ rich in mechanoreceptors and interoceptors that continuously communicate with the central nervous system.
When the nervous system is:
- stressed
- vigilant
- overwhelmed
- dysregulated
Fascial tone increases automatically.
What This Means Clinically
Two practitioners can apply the same technique:
- one experiences profound release
- the other meets resistance
The difference is not skill.
It is nervous system regulation.
How to Influence the Nervous System During Treatment
Fascial tone decreases when the body senses safety through:
- slower pacing
- longer holds
- reduced verbal input
- grounding contact
- predictable rhythm
Regulate first. Release follows.
Ready to Apply These Principles Clinically?
If you want hands-on training that teaches you how to work with fascia instead of forcing tissue, explore our professional education programs:
- Fascia Foundations Course – Fascia Release Dynamic Stretch– Learn the core principles every practitioner must master
- Neuro Fascial Release of Upper & Lower Body Fascia Training – Immediate clinical application
- Advanced Fascia Certification Dynamic Brain Healing – For practitioners who want to specialize and differentiate
Explore Fascia Training Institute Courses
The Fascia Release Formula
Effective fascia release always includes:
- Time over force
- Hydration over stretching
- Regulation over intensity
When these principles are present:
- pain decreases faster
- sessions require less effort
- practitioner fatigue drops
- results last longer
Why This Changes Your Practice
Practitioners who apply these principles consistently:
- become known for results, not effort
- handle complex and chronic cases with confidence
- differentiate themselves in saturated markets
- work smarter — not harder
This is not about adding more techniques.
It is about working with the body instead of against it.

Next Step
If you want to:
- melt fascial tension instead of forcing it
- understand fascia at a systems level
- become the practitioner clients seek out for results
This guide is only the beginning.
Fascia mastery changes everything.
— Fascia Training Institute
Educational content informed by contemporary fascia research, neuroscience, and clinical best practices.
Frequently Asked Questions About Fascia Release
- Why doesn’t fascia respond to deep pressure?
Deep pressure often triggers protective responses in the nervous system. When the brain perceives threat, fascial tone increases. Fascia responds more effectively to slow, sustained input that signals safety.
- Is fascia really contractile?
Yes. Research by Dr. Robert Schleip, Carlos Stecco and colleagues has shown that fascia contains myofibroblasts that can contract and alter tissue tension over time.
- How long does fascia take to release?
Fascial change often occurs within 30–120 seconds when the nervous system is regulated and hydration dynamics are supported.
- Is stretching enough to change fascia?
Stretching alone has a limited impact on fascia. Hydration, slow shear forces, and nervous system regulation play a much larger role in restoring glide and adaptability.
- Why do two practitioners get different results using the same technique?
The difference is rarely technique. It is nervous system regulation, pacing, pressure, and practitioner presence.

